Please excuse my rant and don’t misunderstand my intention. Also, I am not saying that this is ALL relationships, but this is reflective of quite a few relationships between general dentists and specialists.
My intention here is not to throw any specific person, specialty profession, etc under the bus. It is to draw attention to the importance of communication prior to treatment and the importance of communication when things don’t go as expected.
My Specialist Relationship Philosophy
Since the beginning of my dental career I have viewed the general dentist – specialist relationship as a partnership. We should both work in concert to achieve the patients goals in the most conservative manner. This requires a mutual understanding and most importantly communication.
Over the years, I have worked hard on developing these partnerships with various specialists in my area in each discipline. This has led me to not have a ‘rotation’ of specialists that I work with, but go to people. I exclusively refer my patients to these specialty practices. There are, of course, some instances where my patients want another office for insurance or budget concerns.
This nurturing, open communication, and common goal philosophy has led my practice to be able to delivery some pretty exceptional results over the years. It has also allowed each of us to grow – when things aren’t right we work together to make it right. Whether it’s the ‘fault’ of the general dentist or the specialist. To err is human!
Case History
Recently this patient was referred to my office by a local orthodontist for aesthetic enhancement post orthodontics. I always feel it is a great compliment to have a patient referred to me for ‘cosmetics’ by another dentist.

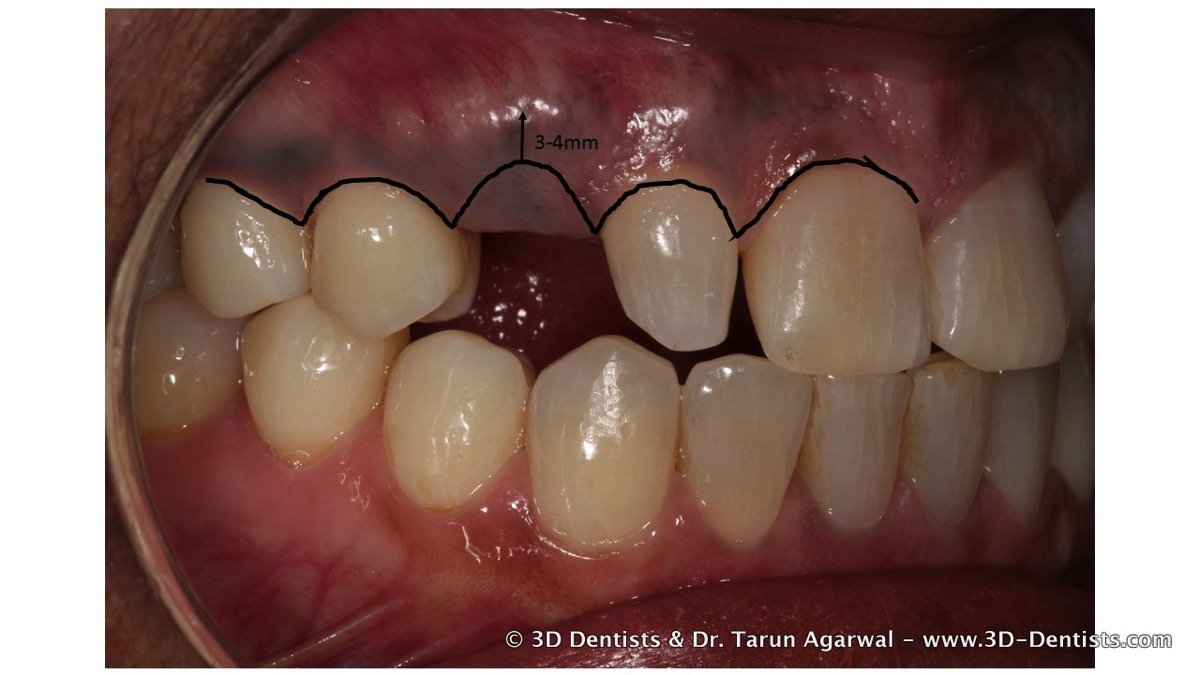
As you can see in the picture the patient would need 4 veneers (##7-10) and an implant in site #6. Site #6 had a impacted retained canine that was ankylosed in place. Since it was ankylosed it would need extraction.
I am not comfortable with removing impacted canines. So i suggested the patient visit my preferred oral surgeon for impacted tooth removal and implant placement in site #6. Based on CBCT data we felt that simultaneous surgery was predictable.
The patient went for the consultation with my preferred oral surgeon. For some reason she chose to have another oral surgeon do her treatment. The unfortunate part was that I learned this when the patient returned to my office for a second consult and the treatment was already done.

With anteriors I prefer to be involved with implant planning to ensure ideal placement based on our final end goal. This is enhanced even more when we are dealing with a congenitally missing tooth. My experience has shown that a congenitally missing tooth requires bone recontouring to develop the gingival shape. This happens since there is no tooth and CEJ to shape the bone – it leaves a flat boney architecture.
So I took my impression for our diagnostic workup – wax ##7-10 and screw retained temporary crown #6.

As it appeared in the mouth the implant was placed at the level of the existing bone and not based on the desired gingival zenith. This was the provisional that was sent back to achieve an aesthetic outcome.

As you can see there is a ridge lap design. This is simply unacceptable from a long term hygiene perspective. So I recontoured the provisional to create an appropriate emergence.

This led to a very unaesthetic look. Below are photos of the provisional on the model. You can clearly see that site #6 is going to be short and squatty and with her smile line will not look very good.


What To Do?
So what can be done to fix this? As an experienced implant restorative dentist who also places most of his own implants – I know the only proper fix in this case is implant removal and new proper, deeper placement.
Using the above photographs and the below photograph I show the patient exactly what I am referring to.

Actually, surgically this case was done extremely well. You can see from this occlusal view of the model the implant is placed exactly through the cingulum and centered mesio-distally. Given that this was done at the time of impacted canine removal, I think the surgery is fantastic. Unfortunately, the implant simply wasn’t placed deep enough.

I recommend to the patient that we consider having the implant removed and a new implant placed. I was more than happy to contact her surgeon (this would be my first interaction with him ever, btw) to go over my findings.
This has happened to me before. Once when I placed my own implants on a missing lateral incisor case and once with a preferred specialist. So I’m no stranger to this. Listen – things happen and the only goal is to try and achieve the best result for the patient.
The Reaction
Unfortunately, the treating surgeon doesn’t see things from my perspective. The surgeon is firm that the implant is placed in the most appropriate position based on the surgical situation and that a deeper placement would be unadvised.
Here is an excerpt from the email exchange….
you and i are unfamiliar with each other’s preferences in terms of the implants placement and it’s restoration, the implant was placed on typical standard fashion based on amount of bone available bucco-lingually and based on vertical deficit of her alveolar bone. as you know she have had orthodontic care and she has short roots and mild to moderate periodontal defect thereby decreasing crown to root ratio to almost 1:1. also you are well aware that deeper the implant they are, probability of developing bone pocket goes up higher. this patient cannot afford to lose any bone due to her short roots and periodontal defect. i would strongly recommend that you consider all these very important factors.
although i do agree that your goal of esthetic is your absolute primary concern but as a reconstructive surgeon, my priority is to assess overall risk and benefit of each surgical procedure. i strongly NOT recommend replacing implant to “bury” it deeper for the pure sense of cosmetic results because further bone loss on her proximal and distal teeth could have negative and unpleasant consequences. my view is current position of the implant is appropriate for her overall bone anatomy.
My assessment of this response is … I’m a ‘reconstructive surgeon’ and you are a general dentist. You weren’t there in surgery and you don’t really know what you are talking about.
It’s possible (and likely) that this is my ego perceiving this.
Here is a pano image of the case.

Why Did This Happen?
So here are my thoughts…..
1. The main mistake here was lack of communication prior to treatment. In defense of surgeon their records indicated a different restorative dentist. However, I’m doubtful any level of collaboration was considered with the restorative dentist of record.
2. I am having a difficult time following the comment regarding existing ‘mild to moderate’ periodontal defect. If there is truly such a periodontal defect then why is implant treatment being done? What was done to alleviate the alleged periodontal defect?
From an aesthetic perspective, this is a diagnosis error. I am confident that the need for a deeper placement was not recognized prior to commencing surgery.
Congenitally missing teeth have a very specific issue when it comes to implant placement. When a tooth is missing the process of eruption doesn’t occur and this affects how the bone is naturally contoured. It is during the phase of ‘passive eruption’ that the bone shrinks back apical to the tooth CEJ. This gives the bone the typical scalloped appearance. When the tooth is congenitally missing the buccal and lingual bone is at the position of the inter proximal bone.
We are taught to place implants at or just below bone level. However, when the bone level is incorrect we need to contour the bone to ideal and then place the implant. This is exactly what has happened in this case.
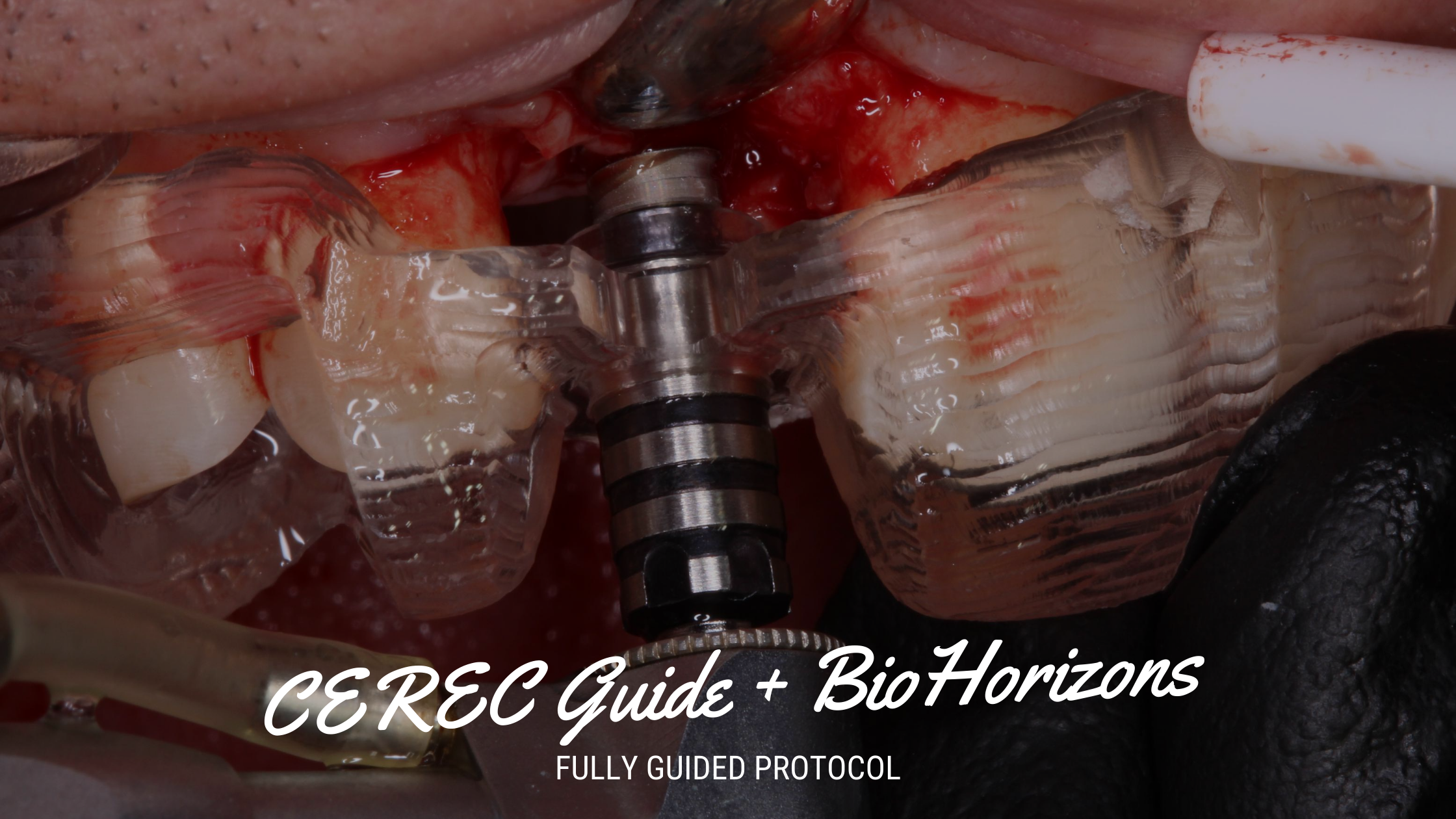
Below is a picture of how one must contour the congenitally missing site prior to implant placement.

Please notice how the bone is NOT contoured from adjacent root to adjacent root. Instead the bone is contoured to create the appearance of a socket shape. This correct contouring is what will ensure that a ‘periodontal defect’ and ‘improper crown to root ratio’ will not be created. With the inter proximal bone height maintained, proper papillae form will also be ensured.
Modern day internal connection implants with a conical connection with platform shift maintains bone quite well around the implant. Given the mesio-distal spacing between #5 and #7 the chances of creating a defect or losing papillae is nominal.
My Loss & Lesson
So here’s where I stand. I’m not in the mood to argue when I perceive someone isn’t willing to listen. So I am refunding the patient their money for the case they paid me. I have lost the time of several consultations, time for records appointment, and laboratory fees associated with wax up and provisional.
At the end of the day I don’t really mind losing money sometimes – it’s the least of my worries. What I dislike is what I feel is ‘bullying’ by specialists and the ‘we know better’ perception. We are all human and make mistakes. Let’s just get it fixed and move forward.
Instead of establishing a partnership this particular surgeon has created an adversarial relationship. No one wins in this scenario. Hopefully, we can all learn from my case – both diagnostically and communication wise. I have my errors in this case and the surgeon has some errors in this case. Who’s at fault is not the goal – the goal is to deliver the best result for the patient.
ULTIMATELY THE PATIENT IS THE LOSER IN THIS CASE.